There are multiple types of knee surgery. An understanding of the specific surgical procedure suggested for you is an essential start. The fear of pain often inhibits the ability to comply with a post-operative rehabilitation program. If this is an issue for you, a discussion about the pain management options available is important in addressing this.
Many people base their knee surgery experience on what family, friends, or neighbours have experienced and this is often not the situation that is going to be experienced by you. That can lead to a misunderstanding and inappropriate expectations. A focused discussion with the surgeon, or the treatment team in general is helpful in clarifying the situation.
Knowledge of the milestone parameters in the recovery process is helpful so that one can assess progress.
Once these aspects are in place, we can get on to the hard work of making the knee work and getting on with our lives. A regular schedule of therapy, home exercise, medication, et cetera is important so that at least for a period of three months or so, we can organise our lives and make the best use of our time.
Differentiating Knee Pain and Hip Pain
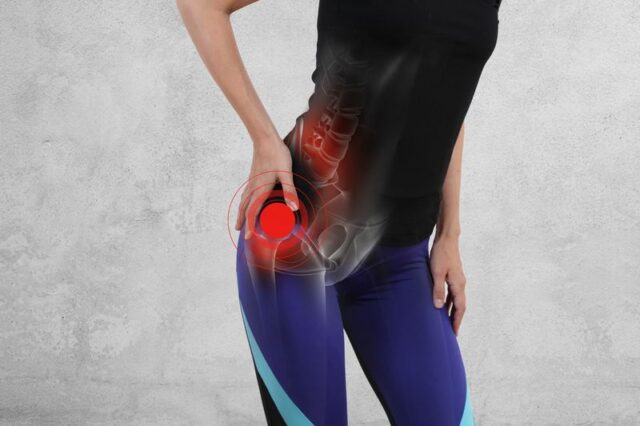
Pain arising from the hip joint itself is usually felt in the groin area, travelling down the thigh, and often into the knee. However, many people attribute pain in the buttock area as arising from the hip. Generally, that is not the case. Pain in this area usually originates in the lumbar spine. As well as the spine, pain in this general area can arise from problems inside the pelvis. Particularly in women. These areas need to be considered.
Looking at the hip region itself, the most common cause would be osteoarthritis. In essence, the joint is worn out – the worn surfaces rubbing against each other. However, other causes may be responsible such as injuries, particularly falls and stumbles. Inflammatory conditions such as rheumatoid arthritis, and occasionally infections. Tumours can be a rare cause. Sometimes, genetic malformations can occur. All of these can lead to pain developing in the hip region.
Knee pain is generally fairly well isolated and can be differentiated from hip pain.
Treatments
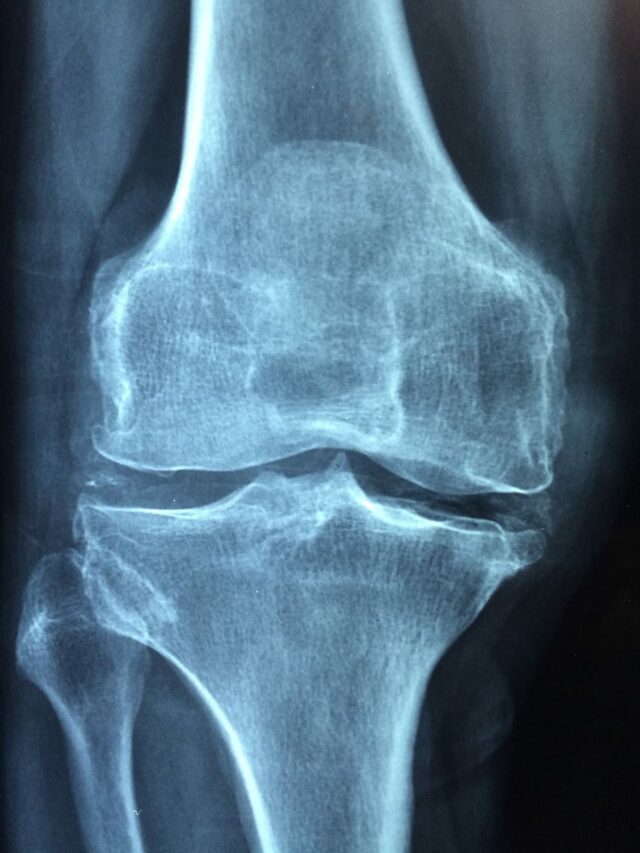
In looking at treatment, the first thing to do is to establish an accurate diagnosis. This is achieved through a full history and physical. Usually, plain x-rays of the knee are a good starting point. Sometimes, an MRI is required and possibly other investigations such as bone scans and blood tests. Many other investigations are possible depending on circumstances. However, let us restrict ourselves to osteoarthritis. Understanding that osteoarthritis is not a dangerous condition, but can be significantly limiting, and restricting to our quality of life, generally, a non-operative approach is adopted initially.
Weight loss, activity limitation, avoiding those activities that would aggravate the knee joint would be a start. We must always remember that the option of using a walking aid is always there. There is no shame in using a walking stick for a little while. Some are quite fashionable! Some people derive significant symptomatic improvement from nutritional supplements such as glucosamine.
It is a little controversial but certainly worth trying.
If these measures are not successful the next step is analgesics, such as Panadol osteo, and if not contraindicated, an anti-inflammatory medication such as Ibuprofen or Meloxicam. As with all medications, care needs to be taken to avoid complications, suggests Professor Lawrence Kohan, an Orthopaedic Surgeon who specialises in knee and hip replacement surgery, about whom you can read more here.
The next step would be a trial of injectables. Intra-articular steroids or a lubricating agent, referred to as visco-supplementation may be considered. Often this option can lead to significant, but temporary improvement in knee mobility and quality of life.
Finally, if these measures still do not lead to an adequate quality of life, then surgical intervention can be considered. There are different types of knee replacements depending on the damage which is present in the knee. This is something to discuss with the surgeon.
When to Have Knee Surgery
People often ask when is the right time to have knee surgery? In my opinion three criteria need to be met.
- The patient must knee experience pain every day;
- The pain is not just a nuisance. The patient plans their day around their knee pain. Such as where to park the car, staging shopping trips, et cetera; and
- Other simpler measures such as those treatment options stated above have been tried, and either had failed or have caused unacceptable side effects.
At this stage, disruption to quality of life is severe enough that the surgical option is likely to lead to an improvement in the quality of life.
Prepare your home for your homecoming after a knee replacement surgery

-
- It is important that you prepare your home before you go for the surgery so that your homecoming is comfortable.
- Rearrange furniture so that you can move around with ease.
- Have a centre where you place all the items that you use frequently and keep it in easy reach.
- Remove any rugs or things from the floor that could cause you to slip.
- Invest in a good and firm chair.
- Install a gripping bar and shower chair in the bathroom.
- Use device for assistance like a sponge with a long handle or a grabbing tool.
It is also important to care for your wound.
-
- Keep the area of the wound clean and dry.
- You will have moderate or severe swelling in the first few months after surgery but it gets mild in around 3 to 6 months.
- Take all medication that has been directed by your doctor.
A full knee replacement is a significant commitment to the treatment process lasting up to one year. On that basis, the starting level of loss of function needs to be bad enough to make the patient feel that the recovery effort required over this period of time is warranted.